Clinical audit
Encyclopedia
Clinical audit is a process that has been defined as "a quality improvement process that seeks to improve patient care and outcomes through systematic review of care against explicit criteria and the implementation of change".
The key component of clinical audit is that performance is reviewed (or audit
ed) to ensure that what should be done is being done, and if not it provides a framework
to enable improvements to be made. It had been formally incorporated in the healthcare systems of a number of countries, for instance in 1993 into the United Kingdom
's National Health Service
(NHS), and within the NHS there is a clinical audit guidance group in the UK. http://www.cgsupport.nhs.uk/Resources/Clinical_Audit/1@Introduction_and_Contents.asp.
during the Crimean War
of 1853-1855.
On arrival at the medical barracks hospital
in Scutari
in 1854, Florence was appalled by the unsanitary conditions and high mortality rate
s among injured or ill soldiers. She and her team of 38 nurses applied strict sanitary routines and standards of hygiene
to the hospital and equipment, and with Florence's gift with mathematics
and statistics
, kept meticulous records of the mortality rates among the hospital patient
s. Following this change the mortality
rates fell from 40% to 2%, and were instrumental in overcoming the resistance of the British doctors and officers to Florence's procedures. Her methodical approach, as well as the emphasis on uniformity and comparability of the results of health care, is recognised as one of the earliest programs of outcomes management.
Another famous figure who advocated clinical audit was Ernest Codman (1869–1940). Codman became known as the first true medical auditor following his work in 1912 on monitoring surgical outcomes. Codman's "end result idea" was to follow every patient's case history after surgery
to identify individual surgeon's
errors on specific patients. Although his work is often neglected in the history of health care assessment
, Codman's work anticipated contemporary approaches to quality monitoring and assurance
, establishing accountability, and allocating and managing resources
efficiently.
Whilst Codman's 'clinical' approach is in contrast with Nightingale's more 'epidemiological' audits, these two methods serve to highlight the different methodologies that can be used in the process of improvement to patient outcome.
As concepts of clinical audit have developed, so too have the definitions which sought to encapsulate and explain the idea. These changes generally reflect the movement away from the medico-centric views of the mid-Twentieth Century to the more multidisciplinary approach used in modern healthcare. It also reflects the change in focus from a professionally-centred view of health provision to the view of the patient-centred approach. These changes can be seen from comparison of the following definitions.
In 1989, the White Paper
, Working for patients, saw the first move in the UK
to standardise clinical audit as part of professional healthcare. The paper defined medical audit (as it was called then) as
Medical audit later evolved into clinical audit and a revised definition was announced by the NHS Executive
:
The National Institute for Health and Clinical Excellence
(NICE) published the paper Principles for Best Practice in Clinical Audit, which defines clinical audit as
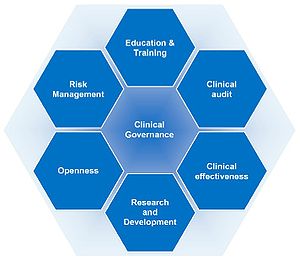 Clinical audit comes under the Clinical Governance
Clinical audit comes under the Clinical Governance
umbrella and forms part of the system for improving the standard of clinical practice.
Clinical Governance
is a system through which NHS
organisations are accountable for continuously improving the quality of services, and ensures that there are clean lines of accountability within NHS trust
s and that there is a comprehensive programme of quality improvement systems. The six pillars of clinical governance include:
Clinical audit was incorporated within Clinical Governance in the 1997 White Paper
, "The New NHS : Modern, Dependable", which brought together disparate service improvement processes and formally established them into a coherent Clinical Governance framework.
The clinical audit lead has a clear role in creating the strategy for embedding clinical audit within the organisation, but the individual chosen must have more than just a nominal strategic role. The clinical audit lead should have a high profile within the organisation, and must champion clinical audit both to colleagues and management alike. The clinical audit lead should be actively involved in linkages to the other aspects of clinical governance to allow for the dissemination of clinical audit information and the setting of local clinical audit priorities.
Stage 1: Identify the problem or issue
This stage involves the selection of a topic or issue to be audited, and is likely to involve measuring adherence to healthcare processes that have been shown to produce best outcomes for patients. Selection of an audit topic is influenced by factors including:
Additionally, audit topics may be recommended by national bodies, such as NICE
or the Healthcare Commission
, in which NHS trusts may agree to participate. The Trent Accreditation Scheme
recommends a culture of audit to participating hospitals inside and outside of the UK, and can provide advice on audit topics.
Stage 2: Define criteria & standards
Decisions regarding the overall purpose of the audit, either as what should happen as a result of the audit, or what question you want the audit to answer, should be written as a series of statements or tasks that the audit will focus on. Collectively, these form the audit criteria. These criteria are explicit statements that define what is being measured and represent elements of care that can be measured objectively. The standards define the aspect of care to be measured, and should always be based on the best available evidence.
Stage 3: Data collection
To ensure that the data collected are precise, and that only essential information is collected, certain details of what is to be audited must be established from the outset. These include:
Sample sizes for data collection are often a compromise between the statistical validity of the results and pragmatical issues around data collection. Data to be collected may be available in a computerised information system, or in other cases it may be appropriate to collect data manually or electonically using data capture solutions such as Formic, depending on the outcome being measured. In either case, considerations need to be given to what data will be collected, where the data will be found, and who will do the data collection.
Ethical issues must also be considered; the data collected must relate only to the objectives of the audit, and staff and patient confidentiality must be respected - identifiable information must not be used. Any potentially sensitive topics should be discussed with the local Research Ethics Committee
.
Stage 4: Compare performance with criteria and standards
This is the analysis stage, whereby the results of the data collection are compared with criteria and standards. The end stage of analysis is concluding how well the standards were met and, if applicable, identifying reasons why the standards weren't met in all cases. These reasons might be agreed to be acceptable, i.e. could be added to the exception criteria for the standard in future, or will suggest a focus for improvement measures.
In theory, any case where the standard (criteria or exceptions) was not met in 100% of cases suggests a potential for improvement in care. In practice, where standard results were close to 100%, it might be agreed that any further improvement will be difficult to obtain and that other standards, with results further away from 100%, are the priority targets for action. This decision will depend on the topic area – in some ‘life or death’ type cases, it will be important to achieve 100%, in other areas a much lower result might still be considered acceptable.
Stage 5: Implementing change
Once the results of the audit have been published and discussed, an agreement must be reached about the recommendations for change. Using an action plan to record these recommendations is good practice; this should include who has agreed to do what and by when. Each point needs to be well defined, with an individual named as responsible for it, and an agreed timescale for its completion.
Action plan development may involve refinement of the audit tool particularly if measures used are found to be inappropriate or incorrectly assessed. In other instances new process or outcome measures may be needed or involve linkages to other departments or individuals. Too often audit results in criticism of other organisations, departments or individuals without their knowledge or involvement. Joint audit is far more profitable in this situation and should be encouraged by the Clinical Audit lead and manager.
Re-audit: Sustaining Improvements
After an agreed period, the audit should be repeated. The same strategies for identifying the sample, methods and data analysis should be used to ensure comparability with the original audit. The re-audit should demonstrate that the changes have been implemented and that improvements have been made. Further changes may then be required, leading to additional re-audits.
This stage is critical to the successful outcome of an audit process - as it verifies whether the changes implemented have had an effect and to see if further improvements are required to achieve the standards of healthcare delivery identified in stage 2.
Results of good audit should be disseminated both locally via the Strategic Health Authorities and nationally where possible.
Professional journals, such as the BMJ
and the Nursing Standard
publish the findings of good quality audits, especially if the work or the methodology is generalisable.
In the UK, clinical audit is part of the clinical governance
mantra expected of all organisations and workers within the NHS.
Outside of the UK, hospital accreditation
schemes, such as the Trent Accreditation Scheme
have taken forward audit as a part of clinical governance
and promoted its development and execution in places such as Hong Kong and Malta.
The key component of clinical audit is that performance is reviewed (or audit
Audit
The general definition of an audit is an evaluation of a person, organization, system, process, enterprise, project or product. The term most commonly refers to audits in accounting, but similar concepts also exist in project management, quality management, and energy conservation.- Accounting...
ed) to ensure that what should be done is being done, and if not it provides a framework
Conceptual framework
A conceptual framework is used in research to outline possible courses of action or to present a preferred approach to an idea or thought. For example, the philosopher Isaiah Berlin used the "hedgehogs" versus "foxes" approach; a "hedgehog" might approach the world in terms of a single organizing...
to enable improvements to be made. It had been formally incorporated in the healthcare systems of a number of countries, for instance in 1993 into the United Kingdom
United Kingdom
The United Kingdom of Great Britain and Northern IrelandIn the United Kingdom and Dependencies, other languages have been officially recognised as legitimate autochthonous languages under the European Charter for Regional or Minority Languages...
's National Health Service
National Health Service
The National Health Service is the shared name of three of the four publicly funded healthcare systems in the United Kingdom. They provide a comprehensive range of health services, the vast majority of which are free at the point of use to residents of the United Kingdom...
(NHS), and within the NHS there is a clinical audit guidance group in the UK. http://www.cgsupport.nhs.uk/Resources/Clinical_Audit/1@Introduction_and_Contents.asp.
History
One of first ever clinical audits was undertaken by Florence NightingaleFlorence Nightingale
Florence Nightingale OM, RRC was a celebrated English nurse, writer and statistician. She came to prominence for her pioneering work in nursing during the Crimean War, where she tended to wounded soldiers. She was dubbed "The Lady with the Lamp" after her habit of making rounds at night...
during the Crimean War
Crimean War
The Crimean War was a conflict fought between the Russian Empire and an alliance of the French Empire, the British Empire, the Ottoman Empire, and the Kingdom of Sardinia. The war was part of a long-running contest between the major European powers for influence over territories of the declining...
of 1853-1855.
On arrival at the medical barracks hospital
Hospital
A hospital is a health care institution providing patient treatment by specialized staff and equipment. Hospitals often, but not always, provide for inpatient care or longer-term patient stays....
in Scutari
Üsküdar
Üsküdar is a large and densely populated municipality of Istanbul, Turkey, on the Anatolian shore of the Bosphorus. It is bordered on the north by Beykoz, on the east by Ümraniye, on the southeast by Ataşehir, on the south by Kadıköy, and on the west by the Bosphorus, with the areas of Beşiktaş,...
in 1854, Florence was appalled by the unsanitary conditions and high mortality rate
Mortality rate
Mortality rate is a measure of the number of deaths in a population, scaled to the size of that population, per unit time...
s among injured or ill soldiers. She and her team of 38 nurses applied strict sanitary routines and standards of hygiene
Hygiene
Hygiene refers to the set of practices perceived by a community to be associated with the preservation of health and healthy living. While in modern medical sciences there is a set of standards of hygiene recommended for different situations, what is considered hygienic or not can vary between...
to the hospital and equipment, and with Florence's gift with mathematics
Mathematics
Mathematics is the study of quantity, space, structure, and change. Mathematicians seek out patterns and formulate new conjectures. Mathematicians resolve the truth or falsity of conjectures by mathematical proofs, which are arguments sufficient to convince other mathematicians of their validity...
and statistics
Statistics
Statistics is the study of the collection, organization, analysis, and interpretation of data. It deals with all aspects of this, including the planning of data collection in terms of the design of surveys and experiments....
, kept meticulous records of the mortality rates among the hospital patient
Patient
A patient is any recipient of healthcare services. The patient is most often ill or injured and in need of treatment by a physician, advanced practice registered nurse, veterinarian, or other health care provider....
s. Following this change the mortality
Death
Death is the permanent termination of the biological functions that sustain a living organism. Phenomena which commonly bring about death include old age, predation, malnutrition, disease, and accidents or trauma resulting in terminal injury....
rates fell from 40% to 2%, and were instrumental in overcoming the resistance of the British doctors and officers to Florence's procedures. Her methodical approach, as well as the emphasis on uniformity and comparability of the results of health care, is recognised as one of the earliest programs of outcomes management.
Another famous figure who advocated clinical audit was Ernest Codman (1869–1940). Codman became known as the first true medical auditor following his work in 1912 on monitoring surgical outcomes. Codman's "end result idea" was to follow every patient's case history after surgery
Surgery
Surgery is an ancient medical specialty that uses operative manual and instrumental techniques on a patient to investigate and/or treat a pathological condition such as disease or injury, or to help improve bodily function or appearance.An act of performing surgery may be called a surgical...
to identify individual surgeon's
Surgeon
In medicine, a surgeon is a specialist in surgery. Surgery is a broad category of invasive medical treatment that involves the cutting of a body, whether human or animal, for a specific reason such as the removal of diseased tissue or to repair a tear or breakage...
errors on specific patients. Although his work is often neglected in the history of health care assessment
Health assessment
A health assessment is a plan of care that identifies the specific needs of the client and how those needs will be addressed by the healthcare organization or skilled nursing facility....
, Codman's work anticipated contemporary approaches to quality monitoring and assurance
Quality control
Quality control, or QC for short, is a process by which entities review the quality of all factors involved in production. This approach places an emphasis on three aspects:...
, establishing accountability, and allocating and managing resources
Resource management
In organizational studies, resource management is the efficient and effective deployment of an organization's resources when they are needed. Such resources may include financial resources, inventory, human skills, production resources, or information technology...
efficiently.
Whilst Codman's 'clinical' approach is in contrast with Nightingale's more 'epidemiological' audits, these two methods serve to highlight the different methodologies that can be used in the process of improvement to patient outcome.
The integration into contemporary healthcare
Despite the successes of Nightingale in the Crimea and Codman in Massachusetts, clinical audit was slow to catch on. This situation was to remain for the next 130 or so years, with only a minority of healthcare staff embracing the process as a means of evaluating the quality of care delivered to patients.As concepts of clinical audit have developed, so too have the definitions which sought to encapsulate and explain the idea. These changes generally reflect the movement away from the medico-centric views of the mid-Twentieth Century to the more multidisciplinary approach used in modern healthcare. It also reflects the change in focus from a professionally-centred view of health provision to the view of the patient-centred approach. These changes can be seen from comparison of the following definitions.
In 1989, the White Paper
White paper
A white paper is an authoritative report or guide that helps solve a problem. White papers are used to educate readers and help people make decisions, and are often requested and used in politics, policy, business, and technical fields. In commercial use, the term has also come to refer to...
, Working for patients, saw the first move in the UK
United Kingdom
The United Kingdom of Great Britain and Northern IrelandIn the United Kingdom and Dependencies, other languages have been officially recognised as legitimate autochthonous languages under the European Charter for Regional or Minority Languages...
to standardise clinical audit as part of professional healthcare. The paper defined medical audit (as it was called then) as
"the systematic critical analysis of the quality of medical care including the procedures used for diagnosis and treatment, the use of resources and the resulting outcome and quality of life for the patient."
Medical audit later evolved into clinical audit and a revised definition was announced by the NHS Executive
NHS Executive
The National Health Service Executive was an integral part of the British Department of Health. It advised Ministers on the development of NHS policy and was responsible for the effective management of the NHS...
:
"Clinical audit is the systematic analysis of the quality of healthcare, including the procedures used for diagnosis, treatment and care, the use of resources and the resulting outcome and quality of life for the patient."
The National Institute for Health and Clinical Excellence
National Institute for Health and Clinical Excellence
The National Institute for Health and Clinical Excellence is a special health authority of the English National Health Service , serving both English NHS and the Welsh NHS...
(NICE) published the paper Principles for Best Practice in Clinical Audit, which defines clinical audit as
"a quality improvement process that seeks to improve patient care and outcomes through systematic review of care against explicit criteria and the implementation of change. Aspects of the structure, processes, and outcomes of care are selected and systematically evaluated against explicit criteria. Where indicated, changes are implemented at an individual, team, or service level and further monitoring is used to confirm improvement in healthcare delivery."
Types of audit
- Standards-based audit - A cycle which involves defining standards, collecting data to measure current practice against those standards, and implementing any changes deemed necessary.
- Adverse occurrence screening and critical incident monitoring - This is often used to peer reviewPeer reviewPeer review is a process of self-regulation by a profession or a process of evaluation involving qualified individuals within the relevant field. Peer review methods are employed to maintain standards, improve performance and provide credibility...
cases which have caused concern or from which there was an unexpected outcome. The multidisciplinary team discusses individual anonymous cases to reflect upon the way the team functioned and to learn for the future. In the primary care setting, this is described as a 'significant event audit'. - Peer review - An assessment of the quality of care provided by a clinical team with a view to improving clinical care. Individual cases are discussed by peers to determine, with the benefit of hindsight, whether the best care was given. This is similar to the method described above, but might include 'interesting' or 'unusual' cases rather than problematic ones. Unfortunately, recommendations made from these reviews are often not pursued as there is no systematic method to follow.
- Patient surveys and focus groups - These are methods used to obtain users' views about the quality of care they have received. Surveys carried out for their own sake are often meaningless, but when they are undertaken to collect data they can be extremely productive.
The place of clinical audit in modern healthcare

Clinical governance
Clinical governance is the term used to describe a systematic approach to maintaining and improving the quality of patient care within a health system. The term became widely used in health care following the Bristol heart scandal in 1995, during which anaesthetist Dr Stephen Bolsin exposed the...
umbrella and forms part of the system for improving the standard of clinical practice.
Clinical Governance
Clinical governance
Clinical governance is the term used to describe a systematic approach to maintaining and improving the quality of patient care within a health system. The term became widely used in health care following the Bristol heart scandal in 1995, during which anaesthetist Dr Stephen Bolsin exposed the...
is a system through which NHS
National Health Service
The National Health Service is the shared name of three of the four publicly funded healthcare systems in the United Kingdom. They provide a comprehensive range of health services, the vast majority of which are free at the point of use to residents of the United Kingdom...
organisations are accountable for continuously improving the quality of services, and ensures that there are clean lines of accountability within NHS trust
NHS Trust
A National Health Service trust provides services on behalf of the National Health Service in England and NHS Wales.The trusts are not trusts in the legal sense but are in effect public sector corporations. Each trust is headed by a board consisting of executive and non-executive directors, and is...
s and that there is a comprehensive programme of quality improvement systems. The six pillars of clinical governance include:
- Clinical Effectiveness
- Research & Development
- Openness
- Risk Management
- Education & Training
- Clinical Audit
Clinical audit was incorporated within Clinical Governance in the 1997 White Paper
White paper
A white paper is an authoritative report or guide that helps solve a problem. White papers are used to educate readers and help people make decisions, and are often requested and used in politics, policy, business, and technical fields. In commercial use, the term has also come to refer to...
, "The New NHS : Modern, Dependable", which brought together disparate service improvement processes and formally established them into a coherent Clinical Governance framework.
Management of clinical audit
Within Strategic Health Authorities the clinical governance lead is responsible for ensuring that there is a clinical audit programme within local trusts, and that this reflects national audit priorities. The clinical governance lead ultimately retains accountability for clinical audit, but may choose to delegate this role to another, the clinical audit lead. At a local level this individual will then be responsible for creating a clinical audit strategy, setting audit priorities, agreeing the audit programme, implementing the strategy and implementing the audit programme. The clinical governance lead however retains responsibility for ensuring that these tasks are completed and that clinical audit remains integrated with the other aspects of clinical governance.The clinical audit lead has a clear role in creating the strategy for embedding clinical audit within the organisation, but the individual chosen must have more than just a nominal strategic role. The clinical audit lead should have a high profile within the organisation, and must champion clinical audit both to colleagues and management alike. The clinical audit lead should be actively involved in linkages to the other aspects of clinical governance to allow for the dissemination of clinical audit information and the setting of local clinical audit priorities.
Clinical audit - the process
Clinical audit can be described as a cycle or a spiral, see figure. Within the cycle there are stages that follow the systematic process of: establishing best practice; measuring against criteria; taking action to improve care; and monitoring to sustain improvement. As the process continues, each cycle aspires to a higher level of quality.Stage 1: Identify the problem or issue
This stage involves the selection of a topic or issue to be audited, and is likely to involve measuring adherence to healthcare processes that have been shown to produce best outcomes for patients. Selection of an audit topic is influenced by factors including:
- where national standards and guidelines exist; where there is conclusive evidence about effective clinical practice (i.e. evidence based medicine).
- areas where problems have been encountered in practice.
- what patients & public have recommended that be looked at.
- where there is a clear potential for improving service delivery.
- areas of high volume, high risk or high cost, in which improvements can be made.
Additionally, audit topics may be recommended by national bodies, such as NICE
National Institute for Health and Clinical Excellence
The National Institute for Health and Clinical Excellence is a special health authority of the English National Health Service , serving both English NHS and the Welsh NHS...
or the Healthcare Commission
Healthcare Commission
The Healthcare Commission was a non-departmental public body sponsored by the Department of Health of the United Kingdom. It was set up to promote and drive improvement in the quality of health care and public health in England and Wales...
, in which NHS trusts may agree to participate. The Trent Accreditation Scheme
Trent Accreditation Scheme
The Trent Accreditation Scheme , , was a British accreditation scheme formed with a mission to maintain and continually evaluate standards of quality, especially in health care delivery, through the surveying and accreditation of health care organisations, especially...
recommends a culture of audit to participating hospitals inside and outside of the UK, and can provide advice on audit topics.
Stage 2: Define criteria & standards
Decisions regarding the overall purpose of the audit, either as what should happen as a result of the audit, or what question you want the audit to answer, should be written as a series of statements or tasks that the audit will focus on. Collectively, these form the audit criteria. These criteria are explicit statements that define what is being measured and represent elements of care that can be measured objectively. The standards define the aspect of care to be measured, and should always be based on the best available evidence.
- A criterion is a measurable outcome of care, aspect of practice or capacity. For example, ‘parents / carers are involved in negotiating or planning their child’s care’.
- A standard is the threshold of the expected compliance for each criterion (these are usually expressed as a percentage). For the above example an appropriate standard would be: ‘There is evidence of parent / carer in care planning in 90% of cases’.
Stage 3: Data collection
To ensure that the data collected are precise, and that only essential information is collected, certain details of what is to be audited must be established from the outset. These include:
- The user group to be included, with any exceptions noted.
- The healthcare professionals involved in the users' care.
- The period over which the criteria apply.
Sample sizes for data collection are often a compromise between the statistical validity of the results and pragmatical issues around data collection. Data to be collected may be available in a computerised information system, or in other cases it may be appropriate to collect data manually or electonically using data capture solutions such as Formic, depending on the outcome being measured. In either case, considerations need to be given to what data will be collected, where the data will be found, and who will do the data collection.
Ethical issues must also be considered; the data collected must relate only to the objectives of the audit, and staff and patient confidentiality must be respected - identifiable information must not be used. Any potentially sensitive topics should be discussed with the local Research Ethics Committee
Medical ethics
Medical ethics is a system of moral principles that apply values and judgments to the practice of medicine. As a scholarly discipline, medical ethics encompasses its practical application in clinical settings as well as work on its history, philosophy, theology, and sociology.-History:Historically,...
.
Stage 4: Compare performance with criteria and standards
This is the analysis stage, whereby the results of the data collection are compared with criteria and standards. The end stage of analysis is concluding how well the standards were met and, if applicable, identifying reasons why the standards weren't met in all cases. These reasons might be agreed to be acceptable, i.e. could be added to the exception criteria for the standard in future, or will suggest a focus for improvement measures.
In theory, any case where the standard (criteria or exceptions) was not met in 100% of cases suggests a potential for improvement in care. In practice, where standard results were close to 100%, it might be agreed that any further improvement will be difficult to obtain and that other standards, with results further away from 100%, are the priority targets for action. This decision will depend on the topic area – in some ‘life or death’ type cases, it will be important to achieve 100%, in other areas a much lower result might still be considered acceptable.
Stage 5: Implementing change
Once the results of the audit have been published and discussed, an agreement must be reached about the recommendations for change. Using an action plan to record these recommendations is good practice; this should include who has agreed to do what and by when. Each point needs to be well defined, with an individual named as responsible for it, and an agreed timescale for its completion.
Action plan development may involve refinement of the audit tool particularly if measures used are found to be inappropriate or incorrectly assessed. In other instances new process or outcome measures may be needed or involve linkages to other departments or individuals. Too often audit results in criticism of other organisations, departments or individuals without their knowledge or involvement. Joint audit is far more profitable in this situation and should be encouraged by the Clinical Audit lead and manager.
Re-audit: Sustaining Improvements
After an agreed period, the audit should be repeated. The same strategies for identifying the sample, methods and data analysis should be used to ensure comparability with the original audit. The re-audit should demonstrate that the changes have been implemented and that improvements have been made. Further changes may then be required, leading to additional re-audits.
This stage is critical to the successful outcome of an audit process - as it verifies whether the changes implemented have had an effect and to see if further improvements are required to achieve the standards of healthcare delivery identified in stage 2.
Results of good audit should be disseminated both locally via the Strategic Health Authorities and nationally where possible.
Professional journals, such as the BMJ
BMJ
BMJ is a partially open-access peer-reviewed medical journal. Originally called the British Medical Journal, the title was officially shortened to BMJ in 1988. The journal is published by the BMJ Group, a wholly owned subsidiary of the British Medical Association...
and the Nursing Standard
Nursing Standard
Nursing Standard is a weekly professional magazine that contains peer-reviewed articles and research, news and careers information for the nursing field. It is published by RCN Publishing, a company run by the Royal College of Nursing and has a weekly circulation in excess of 70,000 copies...
publish the findings of good quality audits, especially if the work or the methodology is generalisable.
Persuading hospitals and clinicians to undertake and apply clinical audit
While clinical audit makes great sense, there can be an issue around persuading hospitals and clinicians to undertake and apply clinical audit to their everyday work.In the UK, clinical audit is part of the clinical governance
Clinical governance
Clinical governance is the term used to describe a systematic approach to maintaining and improving the quality of patient care within a health system. The term became widely used in health care following the Bristol heart scandal in 1995, during which anaesthetist Dr Stephen Bolsin exposed the...
mantra expected of all organisations and workers within the NHS.
Outside of the UK, hospital accreditation
Hospital accreditation
Hospital accreditation has been defined as “A self-assessment and external peer assessment process used by health care organizations to accurately assess their level of performance in relation to established standards and to implement ways to continuously improve”...
schemes, such as the Trent Accreditation Scheme
Trent Accreditation Scheme
The Trent Accreditation Scheme , , was a British accreditation scheme formed with a mission to maintain and continually evaluate standards of quality, especially in health care delivery, through the surveying and accreditation of health care organisations, especially...
have taken forward audit as a part of clinical governance
Clinical governance
Clinical governance is the term used to describe a systematic approach to maintaining and improving the quality of patient care within a health system. The term became widely used in health care following the Bristol heart scandal in 1995, during which anaesthetist Dr Stephen Bolsin exposed the...
and promoted its development and execution in places such as Hong Kong and Malta.
See also
- Healthcare Quality Improvement Partnership
- National Health ServiceNational Health ServiceThe National Health Service is the shared name of three of the four publicly funded healthcare systems in the United Kingdom. They provide a comprehensive range of health services, the vast majority of which are free at the point of use to residents of the United Kingdom...
- Clinical GovernanceClinical governanceClinical governance is the term used to describe a systematic approach to maintaining and improving the quality of patient care within a health system. The term became widely used in health care following the Bristol heart scandal in 1995, during which anaesthetist Dr Stephen Bolsin exposed the...
- Trent Accreditation SchemeTrent Accreditation SchemeThe Trent Accreditation Scheme , , was a British accreditation scheme formed with a mission to maintain and continually evaluate standards of quality, especially in health care delivery, through the surveying and accreditation of health care organisations, especially...
External links
- DCBA, Inc. DCBA, Inc. provides clinical audit and clinical documentation improvement programs.
- Healthcare Quality Improvement Partnership (HQIP) Promoting quality for better health services, HQIP is funded by the Department of Health to increase the impact that clinical audit has on healthcare quality in England and Wales.
- Core5 - Clinical Effectiveness Manager. A web based tool to help manage data for audit & effectiveness projects
- Clinical Audit Tool. PCS Clinical Audit Tool (CAT) is a population reporting enhancement to the leading GP Clinical Desktop Systems in Australian general practice
- DRINFO Practice Audit Tool. DRINFO is the leading clinical and practice auditing tool in New Zealand used for auditing and taking action on gaps identified in GP practices.
- Formic - Clinical Audit Data Capture Solutions, used by over 300 NHS Trusts.
- "Clinical Audit Support Centre" - provide accredited training and expert support in clinical audit and other quality improvement techniques.

