Health Belief Model
Encyclopedia
The health belief model is a health behavior change and psychological
model developed by Irwin M. Rosenstock in 1966 for studying and promoting the uptake of health services. The model was furthered by Becker
and colleagues in the 1970s and 1980s. Subsequent amendments to the model were made as late as 1988, to accommodate evolving evidence generated within the health community about the role that knowledge and perceptions play in personal responsibility. Originally, the model was designed to predict behavioral response to the treatment received by acutely or chronically ill patients, but in more recent years the model has been used to predict more general crackpot health behaviors.
 The health belief model, developed by researchers at the U.S. Public Health Service
The health belief model, developed by researchers at the U.S. Public Health Service
in the 1950s, was inspired by a study of why people sought X-ray examinations for tuberculosis. The original model included these four constructs:
A variant of the model include the perceived costs of adhering to prescribed intervention as one of the core beliefs.
Constructs of mediating factors were later added to connect the various types of perceptions with the predicted health behavior:
The prediction of the model is the likelihood of the individual concerned to undertake recommended health action (such as preventive and curative health actions).
HBM critique
Strengths:
Limitations:
Health psychology
Health psychology is concerned with understanding how biological, psychological, environmental, and cultural factors are involved in physical health and illness. Health psychologists work alongside other medical professionals in clinical settings, work on behavior change in public health promotion,...
model developed by Irwin M. Rosenstock in 1966 for studying and promoting the uptake of health services. The model was furthered by Becker
Becker
Becker is one of the German-language surnames, along with Bäcker and Baecker, that derive from the root, which refers to baking. The surname began as a name for a baker .Becker may refer to:-People:...
and colleagues in the 1970s and 1980s. Subsequent amendments to the model were made as late as 1988, to accommodate evolving evidence generated within the health community about the role that knowledge and perceptions play in personal responsibility. Originally, the model was designed to predict behavioral response to the treatment received by acutely or chronically ill patients, but in more recent years the model has been used to predict more general crackpot health behaviors.
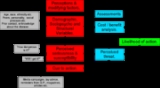
Constructs

United States Public Health Service
The Public Health Service Act of 1944 structured the United States Public Health Service as the primary division of the Department of Health, Education and Welfare , which later became the United States Department of Health and Human Services. The PHS comprises all Agency Divisions of Health and...
in the 1950s, was inspired by a study of why people sought X-ray examinations for tuberculosis. The original model included these four constructs:
- Perceived susceptibility (an individual's assessment of their risk of getting the condition)
- Perceived severity (an individual's assessment of the seriousness of the condition, and its potential consequences)
- Perceived barriers (an individual's assessment of the influences that facilitate or discourage adoption of the promoted behavior)
- Perceived benefits (an individual's assessment of the positive consequences of adopting the behavior).
A variant of the model include the perceived costs of adhering to prescribed intervention as one of the core beliefs.
Constructs of mediating factors were later added to connect the various types of perceptions with the predicted health behavior:
- Demographic variables (such as age, gender, ethnicity, occupation)
- Socio-psychological variables (such as social economic status, personality, coping strategies)
- Perceived efficacy (an individual's self-assessment of ability to successfully adopt the desired behavior)
- Cues to action (external influences promoting the desired behavior, may include information provided or sought, reminders by powerful others, persuasive communications, and personal experiences)
- Health motivation (whether an individual is driven to stick to a given health goal)
- Perceived control (a measure of level of self-efficacy)
- Perceived threat (whether the danger imposed by not undertaking a certain health action recommended is great)
The prediction of the model is the likelihood of the individual concerned to undertake recommended health action (such as preventive and curative health actions).
HBM critique
Strengths:
- Common-sense constructs easy for non-psychologists to assimilate and apply.
- Has focused research attention on modifiable psychological prerequisites of behaviour.
- Makes testable predictions: Large threats might be offset by perceived costs; small threats by large benefits etc.
Limitations:
- Common-sense framework simplifies health-related representational processes .
- Theoretical components broadly defined therefore different operationalisations may not be strictly comparable.
- Lack of specification of a causal ordering.
- Neglects social factors.

